Table of content
- Public Health
- ⛲ Basics of public health
- 👉🏼 Health indicators
- 👨👩👧👦 Family Health
- 🚀 Management of health services
- 💳 Healthcare systems
- 🥼 Practical: Prevention, Projects, Birth & Death Certificates
Member Resources
 Year 4
Year 4 Year 5
Year 5 Year 6
Year 6No access

Public Health
⛲ Basics of public health
Q. In the mission of Public Health, which of the following can be included? (Select all that apply) A. Prevention of injuries B. Assurance of inequity in health C. Prevent epidemics D. Assist communities in recovery after disasters E. Protect against natural disasters
ACD
Domains of Public Health include: 1. ”Statistics + “Science” + “Services” a) Demography b) Biostatistics c) Epidemiology d) Social sciences and behavioral science applied to health. e) Management of social and medical services 2. ”Special”: f) Medical law g) Ethics
- Individual Health: This term denotes a state of comprehensive wellbeing that encompasses physical, mental, and social dimensions. It extends beyond the mere absence of illness or disability.
- Health Status: Health status represents a multifaceted and intricate concept that reflects the overall health of a population. It is evaluated through an amalgamation of various factors
- Security: Ensuring a sense of safety and protection.
- Adequate Income: Having sufficient financial resources for a comfortable life.
- Adequate Home: Access to suitable and stable housing.
- Active Participation in Social Life: Engaging in community and social activities.
- Adequate Social Support: Having a network of friends and family for emotional and practical assistance.
- Healthy Child Development: Influenced by factors such as housing, neighborhood, family income, parental education, physical activity, and genetics.
- Gender: Considering the impact of gender-related factors on health.
- Employment and Working Conditions: Assessing the influence of work-related factors on wellbeing.
- Physical Environment: Evaluating the surroundings and its effect on health.
- Demographic Transition: Studying changes in population demographics over time.
- Changes in Family and Social Structure: Analyzing shifts in family dynamics and societal norms.
5. Healthcare: quality + accessibility
Q. According to Dever's Epidemiological Model, risk factors for health are:
a) Healthcare services b) Healthy consuming habits c) Genetic endowment d) Professional risks e) Media
ACD
Q. According to Dever's model, which of the following are generally accepted as determinants of health?
a) Genetic inheritance b) Religion c) The social environment d) Individual behavior e) The physical environment (natural and built)
ACDE
Health indicators are single measure that are reported regularly for assessing a population's health status and the performance of the healthcare system. These indicators offer actionable insights into various aspects of health, enabling comparisons, monitoring progress, and identifying areas for improvement.
Examples:
- Demographic & Socio-economic: Population, birth rate, total unemployment
- Health status: Disease specific mortality, infant mortality, mobidity, disability
- Health determinants: BMI, BP, Cholest, smoker
- Health intervention: Vaccination, hospital beds+expenditure
- Health promotion (intervention): Policies on health nutrition
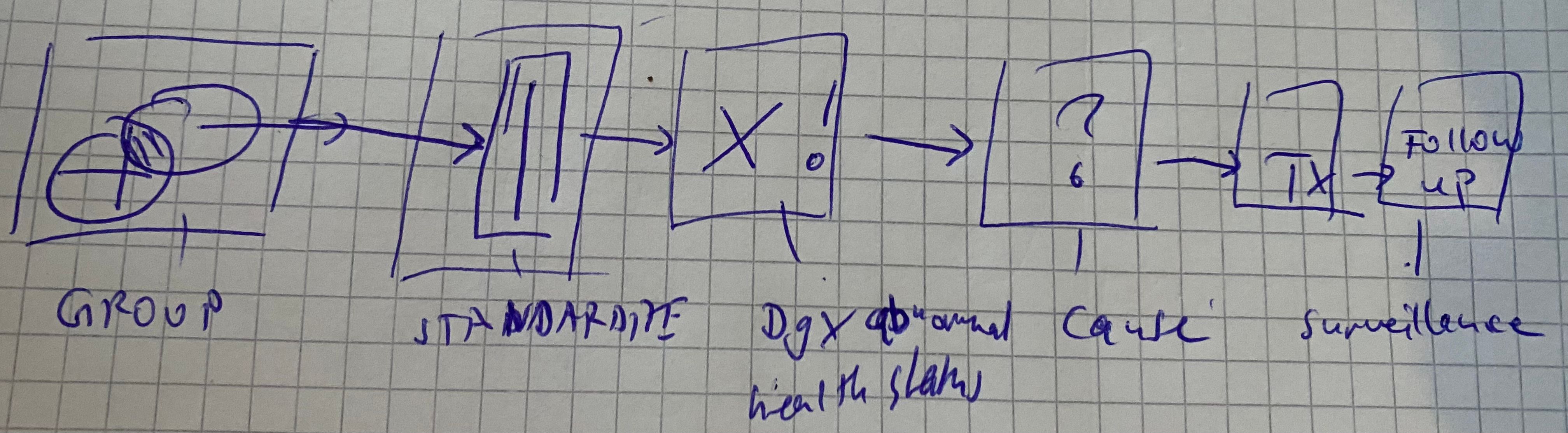
Algorithm for Community Health Diagnosis:
Individual Assessment:
- Identification: Begin by identifying the individual, noting their name, age, and gender.
- Clinic & Diagnostic: Conduct a thorough anamnesis, clinical examination, laboratory tests, and any other relevant examinations. Compare the results with established health norms.
- Individual Health Evaluation: Assess the individual's overall health status.
- Identify Etiology: Determine the underlying causes of any illnesses or health issues.
- Treatment: Implement appropriate treatment strategies, addressing either the root causes or symptomatic relief.
Community Assessment:
- Group Identification: Identify the target group within the community, considering age distribution. Calculate the average age to represent the group's age profile. Also, analyze gender distribution, expressed as the percentage of males and females. Additionally, consider other relevant variables, such as education levels.
- Standard Data Gathering: Collect information in a standardized format. Utilize established processes to calculate various parameters based on the collected data.
- Community Health Diagnosis: Evaluate the overall health status of the community based on the calculated parameters.
- Identify Root Causes: Determine the factors influencing the community's health status.
- Intervention Programs/Tx: Develop and implement intervention programs tailored to the community's needs. These programs should target previously identified risk factors or specific health conditions for which frequency calculations were performed.
- Surveillance: Continuously monitor the community's health status through surveillance mechanisms.
👉🏼 Health indicators
(part of Population’s Structure)

- ⚖️ Average age (arithmetic average)

(14)16-65y (60)
all people that are engaged in a profession + > 14 years (differs from population at emplyment age=16)
A: Economically inactive population includes all persons not engaged in work process such as children up to 14 years, retiring individuals, housewives, persons with disability, students, and unemployed individuals.
⇒ The dependency ratio is the ratio of the economically inactive population to the economically active population.

The rate of replacement is
- the increasing or decreasing percentage of active population,
- the rate of the ratio between persons who become economically active and those who become economically inactive.
Q: Indicators used to describe the age structure of a population are:
(a) Economically active population (b) Population at employment age (c) Masculinity index (d) Femininity ratio (e) Dependency ratio
ABE
typically constructed around 5 year age cohorts or on three ages:
I age = children IInd = adults IIInd = elders
1. Progressive type
2. Stationary type
3. Recessive type
4. Intermediate type (“Growing young”)
transition from ↑high birth and death rates to⇒ ↓low birth and death rates as a country develops from a pre-industrial to⇒ an industrialized economic system.
Q. The Demographic Transition is a model used to represent the transition from:
(a) Industrial to reindustrial period (b) High birth rates to low birth rates (c) Low death rates to high death rates (d) High death rates to low death rates (e) Preindustrial to industrial period
BDE
positive indicator are influenced by marriage & divorces!

Q. Fertility is:
(a) The demographic phenomenon of the frequency of live births in the female population of reproductive age (b) The number of live children per 1000 women of reproductive age (15-49 years) (c) The number of female children (girls) per 1,000 women of childbearing age (15-49 years) (d) The demographic phenomenon of the frequency of live births in a population (e) The number of female children (girls) per 1,000 inhabitants in a population in a period of time
AB
B → Total fertility rate C → GRR D → in a population…? = Natality E → GRR or NRR

- Natality (crude birth rate) = freq. of alive newborns in given population, territory and period of time) per 1000. ⇒ Nr. live newborns / Nr. population x 1000
- Fertility = freq. of alive newborns in female at reproductive age (15-49y) Natality rate = 4x fertility rate (female pop = 50% of population, reproductive age = 50% of femaes
→ if goal is to compare different populations, territoeis → USE FERTILITY (↑specificity)
Total fertility rate = nr of children a woman would have if she would prevail fertility rate at all ages for a particular year ⇒ Nr newborns alive / female at reproductive age (15-49y) x 1000
The total fertility rate in a specific year is defined as the total number of children that would be born to each woman if she were to live to the end of her child-bearing years and give birth to children in alignment with the prevailing age-specific fertility rates. = the average number of children born per woman

Gross Reproduction Rate (GRR): This metric represents the average number of daughters that a woman would give birth to during her lifetime if she was conforming to the age-specific fertility rates for a particular year.
Net Reproduction Rate (NRR): This measure indicates the number of daughters a woman would have in her lifetime, taking into account both age-specific fertility and mortality rates prevailing during a specific year.
i.e. if NNR = 3: 1 woman → after 1 generation: 3 daughters → after 2 generation: 9 daughters
The NRR is less widely used than the TFR, and the United Nations stopped reporting NRR data for member nations after 1998. But the NRR is particularly relevant where the number of male babies born is very high.
a) Demographical: Population structure b) Medical and Biological: Sterility, sexual hygiene c) Social: Length of educational period, women's labor force participation d) Migration: Consider the impact of migration on fertility e) Legislative: Family planning and family protection policies f) Subjective: Individual beliefs and preferences g) Traditional, Cultural, and Religious: Cultural and religious factors h) Urbanization
ABCD
industrialized ⇒ 2.1 children/woman
developing ⇒ ↑ 2.5 - 3.3 ( due to ↑mortality)
globally ⇒ 2.33

“The total fertility rate is generally computed by summing up the age-specific fertility rates defined over a five-year interval. Assuming there are no migration flows and thatmortality rates remain unchanged, a total fertility rate of 2.1 children per woman generates broad stability of population: it is also referred to as the “replacement fertility rate”, as it ensures replacement of the woman and her partner with another 0.1 children per woman to counteract infant mortality”

Q. *Fatality:
- A. Represents the death rate caused by a disease per 100 patients diagnosed with that disease
- B. Is also called proportional mortality
- C. Represents the frequency of deaths per 1000 inhabitants
- D. Represents the average number of years a person is expected to live
- E. Represents the frequency of diseases per 1000 inhabitants
A
= proportional mortality
indicates frequence with which a specific cause of death occurs among the total number of death ⇒ RANKS of death 📷
Q. Lethality:
A. Represents the share of deaths of a certain cause out of the total number of deaths
B. Represents the frequency of diseases per 1000 inhabitants
C. Represents the frequency of deaths per 1000 inhabitants
D. Is also called proportional mortality
E. Allows the establishment of ranks in mortality
ADE
- Economic factors (socio-economic development)
- National income distribution
- Age structure within a given population
- Environment-related factors
- Educational and technological skills
Q. Among the factors that influence mortality are:
A. Gender structure of the infant population B. Existence of primary care services C. Technological skills D. Level of education E. National income distribution
BCDE

- Mortality rates are essential for assessing population health.
- Reveal health issues serve as a foundation for setting healthcare priorities.
- Mortality rates guide healthcare planning and strategy development.
- They aid in resource planning for healthcare.
- Mortality rates enable the evaluation of medical activities within the healthcare system.
Developed Countries | Developing Countries | |
Mortality in Infants | Low ↓ | High ↑ |
Life Expectancy | High ↑ | Low ↓ |
Mortality in Aged People | High ↑ | |
Age Specific Mortality | J-like curve 📷
(advanced mortality pattern) | U-like curve 📷
(primary mortality pattern) |
Death-Cause Specific Mortality | Chronic degenerative diseases come first in rank | Respiratory, infectious, maternal and infant diseases and digestive diseases come first in rank |
Intermediate Pattern | Acute infectious diseases lead to decreasing mortality rates and chronic degenerative diseases lead to increasing mortality rates (i.e. Romania) |
Q. The mortality dynamics in developing countries:
- A. Describe a "U" curve.
- B. Shows high death rates at the third age.
- C. Shows high death rates at the first age.
- D. Is due to the increase prevalence of chronic diseases.
- E. Is due to the low prevalence of chronic diseases.
BD
Q. True affirmations about advanced mortality type:
- A. Is specific in developing countries
- B. Deaths occur more frequently over the age of 40
- C. Is dominated by infectious diseases
- D. Is dominated by maternal & infant diseases
- E. Is specific in developed contries
BE
Q. What affirmations are true about primary mortality type:
A) It is specific for developing countries B) The graphic representation describes a “J” like curve C) It is dominated by infections and respiratory diseases D) It is dominated by chronic diseases D) Deaths occur more frequently in childhood
ACE
Q. "Advanced" morbidity type:
A) Is characterized by numerous infectious endemic diseases B) Is a consequence of demographic transition C) Is characteristic for developed countries D) Is characteristic for underdeveloped countries E) Is characterized by numerous chronic diseases
BCE
Nr. Infant-Deaths (≤1y) per 1000 live births
i.e. if infant mortality = 3 ⇒ out of 1000 births 3 infants die
“The rate of infant mortality in a given region is the total number of newborns dying under one year of age divided by the total number of live births during the year, then all multiplied by 1,000. The infant mortality rate is also called the infant death rate (per 1,000 live births).”
Q. Infant mortality rate:
A) Indicates the level of development of a country. B) Represents the number of infant deaths per 1,000 live newborns. C) Is typically higher in less developed countries. D) Is lower in developed countries. E) Represents the number of infant deaths within the total population.
ABC

- Socio-economic (mother + family)
- New born characterisitics Newborn range, Low weight at birth
- Healthcare system
- Developed vs. developing country (socioeconomic system)
Mother's instruction level, Mother's education, Social and economic level of the family
Population accessibility to healthcare services, quality of diagnostics
Nourishment, Social protection system
Q. Risk factors for infant mortality are:
A) The rank of the newborn B) Mother's education C) High natality in a population D) Healthcare system E) Social protection system
BDE (+/- A: if typo and “range of the newborn” is meant)
- Infant Mortality Rate (IMR) Decline: IMR significantly decreased from 65% in 1990 to 29% in 2017 worldwide.
- Disparity Between LDCs and MDCs: IMR remains significantly higher in Less Developed Countries (LDCs), at a rate 17 times higher than More Developed Countries (MDCs).
- Neonatal Deaths: In 2017, infant deaths accounted for 75% (4.1 million) of all deaths among children under five, with 45% of these being neonatal deaths.
- Daily Newborn Deaths: Shockingly, approximately 7,000 newborns lose their lives every day worldwide.
- Regional Disparities: The risk of a child dying before their first birthday is six times higher in the World Health Organization (WHO) African Region compared to the WHO European Region.
Death of woman while pregnant or within 42d of termination of pregnancy
→ from any cause related/aggrevated by pregnancy or management→ but NOT from ACCIDENTAL or INCIDENTAL causes
(irrespective of: duration, site)
Q. Maternal mortality rate: (a) Represents the death of a woman who has one child or more. (b) Includes deaths during pregnancy by any cause. (c) Tends to be higher in Less Economically Developed (LED) countries. (d) Is a positive demographic indicator. (e) Is a health indicator that reflects the development of the healthcare system
CE
Maternal mortality ratio: The number of maternal deaths during a specific time period per 100,000 live births that occurred during the same time period.
Maternal mortality rate: The number of maternal deaths during a specific time period per 100,000 women of reproductive age who were alive during the same time period.
Direct Obstetric Deaths | Indirect Obstetric Deaths | |
Definition | Deaths resulting due to obstetric complications of the pregnant state (pregnancy, delivery, and postpartum) as a cause of interventions, omissions(neglect), incorrect treatment, or from a chain of events resulting from any of the aforementioned. | Resulting from previously existing disease, or diseases that have developed during the course of pregnancy, and which are not due to direct obstetric causes but aggravated by physiological effects of pregnancy. |
Difference | Direct obstetric deaths are caused by iatrogenic or negelected complications of the pregnant state, | indirect obstetric deaths are caused by diseases aggravated by pregnancy. |
Examples | - Hemorrhage, pre-eclampsia, eclampsia
- complications of abortion, anesthesia, cesarean section
| - deaths due to aggravation of an existing cardiac or renal disease
|

In Developing Countries:
- Hemorrhage
- Toxemia
In Developed Countries:
- Hemorrhage
- Infections (puerperal)
- Accidents during delivery
- Asepsis
- Fluid management
- Blood transfusion
- Better prenatal care
Q. Natural movement of a population: (a) Has a main influence on population's structure (b) Consists of natality, fertility, and mortality (c) Has 3 components: positive, negative, and migration (d) The negative component includes maternal mortality (e) The positive component is influenced by the rate of divorces
ABDE
TOTAL ILLNESSES know at
- specific time
- specific region/terriotory
- also included are: trauma, indox, injuries, burnings
Morbidity refers to the collective occurrence of illnesses within a specific population during a defined period, typically a calendar year. It encompasses the documented instances of disease manifestation, signifying a shift in an individual's health status. In statistical terms, the unit of observation is the "disease" itself or, in a longitudinal perspective, the affected individual.
“ a) General morbidity: Incidence and prevalence at a given moment or period. b) Morbidity on contingents: Number of persons grouped based on the same characteristics (..). c) Successive morbidity: Estimated by health status survey. d) Morbidity with temporary incapacity for work. e) Morbidity with permanent incapacity for work. f) Hospitalized morbidity.”
Q. Indicators for studying morbidity are:
A. Successive morbidity
B. Structure of incidence
C. Specific mortality
D. Incidence
E. Hospitalized morbidity
ADE
(D = general)
🥇 Respiratory diseases
🥈 Digestive diseases
🥉 Diseases of the nervous system and sensory organs
- Accessibility
- Addressability
- Quality of diagnostic
“Incidence should be considered the real frequency of illnesses only in those specific areas where the three conditions are optimal, even though 10% of illnesses remain unknown.”
General Morbidity Incidence: “The frequency of new cases that are registered in an area in a specific period of time (month, trimester, year) by all the healthcare services. When the incidence is calculated only illnesses which were first diagnosed are taken under consideration. The acute illnesses, which are cured and then reappear (but do not relapse) are considered as NEW CASES. When more diseases are detected in one patient, each of them will be coded. It is the (number of new cases of disease /total number of illnesses) X 100. It will show the frequency of the diseases, and with this, we can obtain the morbidity ranks.”
Q. Incidence: a) Takes under consideration all the diseases existing in a population. b) Takes under consideration only the illnesses which are newly diagnosed. c) The acute illnesses which are cured once and reoccur are not taken into consideration. d) If a person has more diseases, the new diagnosed diseases are reported in only one case e) If a person has more diseases newly diagnosed, each one of them is reported separately.
BE
MOMENT prevalence = All illnesses present at a moment (last day of the month)
PERIODIC prevalence = All illnesses present in a period (trimester, year)
Q. * Prevalence refers to:
A. All illnesses existing at a specific moment, regardless of the date of diagnosis. B. Percentage of diseases of a certain cause. C. New cases of disease in a year/territory. D. Number of deaths in a year/territory. E. Number of deaths of a certain cause.
A
Category | Primitive Type | Advanced Type |
Diseases | Infectious, Parasitic, acute digestive | Chronic CV and metabolic diseases |
Malnutrition | High prevalence of protein-calorie malnutrition | Occurrence is lower |
Socio-Economic Status | Typically found in undeveloped countries ⇒ CHILDREN! | Typically found in developed countries
⇒ ELDERY! |
Q. Advanced morbidity types:
A) Is characteristic for less developed countries. B) Is characteristic for developed countries. C) Is characterized by numerous infectious endemic diseases. D) Is characterized by numerous chronic diseases. E) It is not a consequence of demographic transition.
BD
👨👩👧👦 Family Health
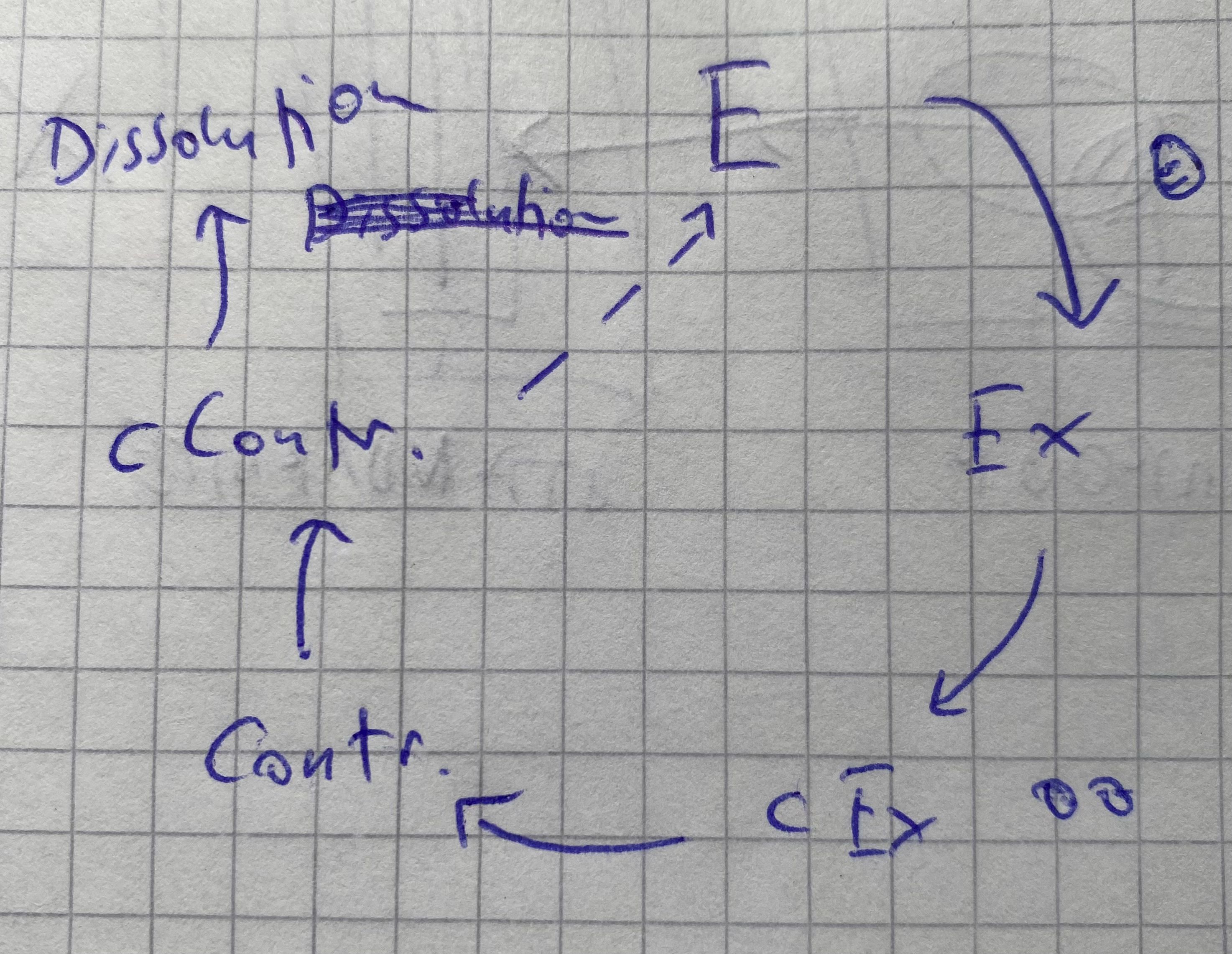
a) Entry into marriage: Wedding. b) Family extension: Birth of the first child. c) Complete family extension: Birth of the last child. d) Contraction: First child gets married and leaves home. e) Complete contraction (”empty nest”): Last child gets married and leaves home. f) Dissolution: One of the spouses dies.
Demographic determinants:
- Birth rate
- Mortality
- Marriage rate
- Marital dissolution
Socio-economic determinants:
- Socio-economic status of the country
- Average income per family member
- Urbanization and industrialization
Cultural determinants:
- Education
- Cultural level of a given population
Q. Socio-economic determinants that influence the family cycle are:
- A. Industrialization
- B. Mortality
- C. Nuptiality
- D. GDP of the country
- E. Cultural level
AD
In recent years, we've witnessed a decline in mortality rates, leading to more eligible individuals and elderly survivors. This has prolonged the family cycle, extending it by approximately 13 years compared to the early 20th century. Marital dissolution, which was once primarily due to the death of wives related to pregnancy and childbirth, now more commonly occurs following the death of husbands. These changing demographics emphasize the evolving nature of population dynamics and their impact on society.
- 1) 🎓 Family structure (age, education, occupation)
- 2) ↔️ Family size
- 3.) ♻️ Family cycle, environment + lifestyle
- MODERN ("NUCLEAR”) family: Husband + wife +/- children
- CLASSIC (”ENLARGED”) family
- VERTICALLY enlarged family: husband + wife +/- children + 1 of spouse’s parents
- HORIZONTALLY enlarged family: husband + wife +/- children + 1 of spouse’s siblings
- HORIZONTAL + VERTICAL: husband + wife +/- children + 1 of spouse’s siblings/parents

Q. Demographic indicators used to assess family health are:
(a) Age. (b) Nationality. (c) Family size. (d) Family cycle. (e) Education.
ACDE
- Frequency of risk factors in the family
- Frequency of diseases in the family
- Number of diseases in a family
- Identification of families with high risk for disease
APGAR code with a maximum score of 10
- If anything wrong happens, I can turn to my family for help.
- My family shares and embraces problems with me.
- My family spends quality time together.
- My involvement in new activities is accepted and supported by my family.
- My family responds to my feelings (love, anger, rage).
- Healthy family (8-10 points)
- Troubled family (6-7 points)
- Family at risk (< 6 points)
→ Answers: always = 2pt; sometimes = 1pt.; never = 0 points → Interpretation
- Consider the financial aspects and disease's impact on a family's health.
- The doctor should show interest in the economic factors that influence family health.
- Take note of the medical terminology and key terms for the exam.
🚀 Management of health services
- External changes (freq. & impact)
- ↑ of Health system complexity
- ↑Time period betw. decision taking time & results archieving time
Iterative means involving repetition and refinement of a process or idea over time, with the goal of improving it with each repetition.
- Structural
- Formal
- Long term: Departments
- Short term: Working groups
- Long-term: Establish permanent structures in different departments
- Short-term: Form task-oriented working groups that dissolve after achieving their goals (e.g., emergencies, outbreaks)
- Informal
- informal relations
- “opinion leaders”
- Informal relations within an organization, including friends, professional associations, and informal working groups.
- "Opinion leaders" who hold influence within the organization, even without formal authority.
- These informal networks play a crucial role in shaping organizational dynamics and decision-making processes.
- They can impact information flow, knowledge sharing, and the adoption of new ideas or practices.
- It is important to understand and leverage these informal networks for effective organizational management and change implementation.
- Functional
- Functions
- Services
- Products
- Functions: Clinical laboratory, X-ray, Pharmacy
- Services: Emergency room, Waiting rooms
- Products: Maternity, Diabetes centers
- Recruiting employees (hiring process)
- Selection of future employees
- Allotment of personnel in existing structural posts
- Personnel training to enhance job performance
- Employee counseling for career advancement opportunities
- Establishment of criteria for employee compensation and benefits
- Employee retirement, transfer, or termination procedures
- Simple delegation: Used in small units for simple tasks.
- Authorization: Limited mandate for solving specific tasks.
- Commission: Provides more freedom.
- Temporary passing of power to another employee: Occurs during legal holidays, study holidays, or sick leave. It delegates both responsibility and authority.
- Principles of authority delegation:
- Responsibility cannot be delegated except for temporary transfer of power.
- Responsibility is proportional to the delegated authority.
- Delegation aims to gain experience, increase professional level, demonstrate incapacity or ineffectiveness of subordinates.
- Basic rules in delegation of authority:
- Precisely and clearly establish objectives and tasks.
- Motivate the delegation clearly.
- Ensure resources (human, financial, and time) are in accord.
- Formulate responsibilities precisely.
- Give a degree of "liberty of action" to the person delegated with authority.
- Provide a system for control and efficient information feedback.
✅ Authorities that can be delegated | ❌ Authorities that can Ø be delegated |
Routine tasks | Difficult tasks |
Tasks which can be carried out just as well or better by others | A subordinate's evaluation |
Tasks that require special training | A subordinate's advancing or rewarding proposals |
Tasks that target the increase of a subordinate's professional level | Authorities linked with prestige and reputation of the manager |
Q. Tasks that can be delegated, are: A. difficult tasks B. simple tasks C. tasks which require special training D. tasks which can be as well or better carried out by other persons E. subordinate's evaluation
BCD
- Autocratic Style: This leadership style involves using a command and execution approach, where subordinates are motivated through rewards or sanctions. Communication is primarily one-directional.
- Participative Style: This leadership style involves consulting subordinates and involving them in decision-making. Communication flows both ways, vertically and horizontally, resulting in a more team-oriented approach.
- Laissez-Faire Style: This leadership style is characterized by granting a high level of autonomy to subordinates, even for actions outside the group. It allows for individual freedom and initiative.
- Setting standards of time, quality, and quantity.
- Measuring results.
- Comparing results with the standards.
- Applying necessary changes to achieve the standards.
- Reactive control: evaluation, comparison of standards, identifying flaws, implementing corrective measures, evaluating new results
- Control in real time: requires a robust information system
- Proactive control: feed-forward, preventative actions
Categories | Technical Abilities | Human Abilities | Conceptual Abilities |
Characteristics | Specific to the type of coordinated activity → Task oriented | Essential for the manager to work with individuals or groups. | About seeing the links between complex situations, having a view of the future, and to see all parts as an entity. |
Skills | Reading and interpreting a financial report, writing a report, or making a proposal on a subject. | Understanding and taking into consideration the attitude, perception, or the subordinate's sentiments in order to gain their trust. | Seeing the consequences of their own actions. |
Importance | Important for lower-level managers, but less important for higher-level managers. | Equally important for all levels of managers. | Very important for top managers, but can also help lower-level managers achieve the integration of their units in the system. |
Q. Manager's abilities can be: A. Conceptual B. Informational C. Technical D. Interpersonal E. Human
ACE → 📷
🤝 INTERPERSONAL
- representative in social acitivies
- leader of department
- link with other department
📢 INFORMAL
- source + disseminator of information
- monitoring of information
- “spokesman” (speaks in name of the company)
👉🏽 DECISIONAL
- entrepreneurial (searches new ideas to improve activity)
- mediator in conflicts
- resource distributer
- negotiator with other organizations
Q. Interpersonal roles of managers are: a) Distributor of resources b) Mediator of conflicts c) Link d) Representative of his organization e) Leader
CDE
Q. Authority sources in management are: A. Friendly relationship with the subordinates B. Competence C. Leadership D. Hierarchy E. Charisma
- service = patient oriented
- constant quality improvement
- employee satisfaction
- groups of interest (that are affected by results)
- Social or physical aspect
- Organizational values
- Basic assumptions
- Mechanisms of measuring and controlling employee activity (same for every employee!)
- Leader's reaction in various situations
- Leader as a role/”raw” model
- Leader’s benefit partition criteria
- Leader recruitment selection, and promotion criteria
💳 Healthcare systems
Health Service | Characteristics | 👍🏼 Advantages | 👎🏼 Disadvantages |
💸 NHS
(Denmark, Finland, Iceland, Norway, Sweden, Greece, Italy, Portugal, Spain and UK)
aka Beveridge type | - Financed through general taxes,
- government-controlled, benefits of state budget,
- there is a private sector,
- free access for all citizens ⇒ full coverage of the population, involvement of state authorities in administrative decisions,
- payment to doctors according to the number of patients on their lists (capitation), some services require co-payment | Positive impact on health status, not very expensive for the population, also full coverage | Patients have to wait their turn for specific procedures, lack of doctors' stimulation, too much bureaucracy |
🏗️ SIHS
(Austria, France, Holland, Germany and Belgium)
aka Bismark type | - Financed through compulsory contribution of employees and employers, according to income and general taxes, broad, although not full coverage (unemployed patients are not insured),
- agencies are in administrative charge, agencies sign contracts with hospitals and with family doctors/general practitioners as to the procedures provided to patients,
- the contracts set forth the tax per procedure (when doctors are involved) or are based on the global budget (for hospitals) | High medical standards | Expensive - the most expensive in Europe, administrative costs are high, generates high induced consumption which can lead to pervert situations such as:
- moral risk (a free procedure leads to a demand that exceeds the supply),
- adverse selection (expensive groups will not be satisfied) |
🏰 SOHS
(Central and Eastern Europe)
aka Semasko type
| - Financed through state budget, - state controlled through central planning system, health services owned exclusively by the state, medical staff employed by the state,
- full coverage of the population,
- no private sector | Full coverage of the population | Lack of initiative and competition, medical staff work as functionary, low finance, ineffective, low impact on health status |
Q. The National Health Service System (NHS):
A) Is financed through general taxes B) Is financed through compulsory contributions by employers and employees C) Assures full coverage of the population with medical services D) The population's coverage with medical services is large but not complete E) It is controlled by independent agencies
AC
Q. The Social Health Insurance System: A. ensures full coverage of the population with medical services B. is financed through general taxes C. it generates long waiting lists D. is also called the Bismark Type System E. it generates high administrative costs
DE
Q. The National Health System (NHS):
A. The population's coverage with medical services is large but not complete.
B. It is controlled by the government.
C. It is financed through general taxes.
D. It is financed through compulsory contributions from employers and employees.
E. It ensures full coverage of the population with medical services.
BCE
- Full coverage of the population
- Full accessibility
- Responsiveness to the specific needs of the population
- Equity
- Freedom of choice
- Efficiency
- Broad acceptance
- Accountability of the state for the health status
Q. An adequate healthcare system should have:
A. Efficiency B. Freedom of choice C. Full coverage of population with services D. Broad coverage of population with services E. Full accessibility
ABCE
- Equal chances
- Ethical actions in health policies
- Involvement of the population
- Health promotion and disease prevention
- Primary health care as a priority
- Inter-sectorial action
- International cooperation
🥼 Practical: Prevention, Projects, Birth & Death Certificates
Type | Aim | Method |
Primary Prevention | Prevent disease or injury before it occurs | Prevent exposure to hazards that cause disease or injury, alter unhealthy or unsafe behaviors that can lead to disease or injury, increase resistance to disease or injury. |
Examples | Legislation and enforcement to ban or control the use of hazardous products, education about healthy and safe habits, immunization against infectious diseases. | |
Secondary Prevention | Reduce the impact of a disease or injury that has already occurred | Detect and treat disease or injury as soon as possible to halt or slow its progress, encourage personal strategies to prevent reinjury or recurrence, implement programs to return people to their original health and function to prevent long-term problems. |
Examples | Regular exams and screening tests to detect disease in its earliest stages, daily, low-dose aspirins and/or diet and exercise programs to prevent further heart attacks or strokes, suitably modified work so injured or ill workers can return safely to their jobs. | |
Tertiary Prevention | Reduce the impact of an ongoing illness (chronic) or injury that has lasting effects | Help people manage long-term, often-complex health problems and injuries, in order to improve as much as possible their ability to function, their quality of life, and their life expectancy. |
Examples | Cardiac or stroke rehabilitation programs, chronic disease management programs, support groups that allow members to share strategies for living well, vocational rehabilitation programs to retrain workers for new jobs when they have recovered as much as possible. | |
Quaternary Prevention | Identify patients at risk of over-medicalization, protect them from new medical invasion, suggest interventions that are ethically acceptable | - |
- All the preventive medical measures taken by the healthcare network to identify potential illnesses and risk factors in the population at an early stage.
- These measures target individuals who are presumed to be in good health and should not be confused with follow-up activities.
- Active prevention includes compulsory medical examinations at different stages of life and occasional check-ups.
- It also emphasizes the active role of individuals in adopting healthy lifestyle habits and taking responsibility for their own health.
- Prevention for inherited, genetic, or consisting of specific weaknesses health issues
- Prevention of contracting lifestyle diseases by living a healthy lifestyle and overcoming an already diagnosed lifestyle disease
- Prevention of suspected health conditions where no medical diagnosis could be established, ensuring that the suspected issue is less likely to develop
- Prevention of a “medically diagnosed health issue” from getting worse while supporting general health and well-being to be able to overcome that health condition
- Prevention of chronic diseases from becoming worse
prenuptial = pre-marriage
= Medical exam for a couple before it gets married:
- physical exam
- psych exam
- Chest XRAY
- Syphilis testing (VDRL)
Q. Compulsory medical examinations for prenuptial medical certificate (PMC)
A. X-ray examination of the thorax
B. Psychiatric examination
C. Syphilis screening
D. Physical examination
E. HBs antigen testing
ABD
- Definition/Planning:
- Needs assessment
- Goal and objectives (targets) predefinition
- Identification of activities, resources, partners, financing, team, and schedule
- Implementation:
- Activities and management (human resources, financing, technique)
- Public relations strategy and communication
- Evaluation process feedback and community involvement
- Evaluation:
- Measurement of indicators
- Impact on community and organization
- Documentation description and financial records
- Closure of bank accounts
Q. *Regarding the goal of a project, the following affirmations are true: A. It should be SMART defined B. It is something concrete C. It should have a deadline D. It should be revisited periodically E. It must change along the project
A
Q. The objective of a health project is: A. Achievable B. Timeless C. Short D. Measurable E. Specific
ADE
Feature | Live Newborn | Dead Newborn |
Country, County, Town | ✔️ | ✔️ |
Place of Birth | ✔️ | ✔️ |
Who Assisted the Birth | ✔️ | ✔️ |
Type of Birth | ✔️ | ✔️ |
Single/Multiple | ✔️ | ✔️ |
Weight at Birth | ✔️ | ✔️ |
Height | ✔️ | ✔️ |
Pregnancy Time (in weeks) | ✔️ | ✔️ |
Newborn's Legitimacy | ✔️ | ✔️ |
Causes of Death | ❌ | ✔️ |
Parent's Data | ✔️ (mother’s) | ✔️ |
Marital Status | ✔️ | ❌ |
- Medical certified ascertaining birth: A medical act with forensic implications, used for cases such as infanticide, abandonment, establishing paternity, or investigating infant deaths. It differs from a birth certificate, which is a civil status document.
- Release procedure: Only health facilities and attending doctors can issue the medical certificate. In Romania, births must be attended by a doctor and midwife in a health facility. If a birth is attended only by a midwife or is unassisted, the family doctor must examine the mother and newborn within 24 hours and issue the medical certificate.
Q. The medical certificate of birth:
- A. Can be completed by a nurse.
- B. It is completed in the first 24 hrs. after ascertaining the birth with an alive newborn.
- C. Is completed only by the doctor who assisted the birth.
- D. Is completed by the doctor who ascertains the birth.
- E. Is the same as the birth certificate.
BD
… 24hours … real signs of death (i.e. cadaver lividity).
- Violent death: includes accidents, suicides, and homicides
- Unknown cause of death
- Suspect cause of death: includes sudden death, inpatient death, etc.
- Country, county, town
- First name, last name, gender
- Year, month, day: birth and death
- Marital status + Education
- Causes of death

